Have you ever noticed your back or neck pain gets worse during stressful times? You’re not imagining it. Stress and pain are closely connected through the brain–body relationship, and understanding this connection can help you better manage chronic pain.
At Kansas Pain Management, we often see patients whose pain flares up not just from physical causes, but also from stress, anxiety, and poor sleep. The good news is that once you understand why this happens, you can take steps to control it.
How Stress Affects the Body
When you experience stress, your body activates the “fight or flight” response. This leads to:
- Increased muscle tension
- Release of stress hormones like cortisol
- Heightened sensitivity in the nervous system
- Reduced ability to relax and recover
While this response is helpful in short-term situations, chronic stress keeps the body in a constant state of tension, which can worsen pain.
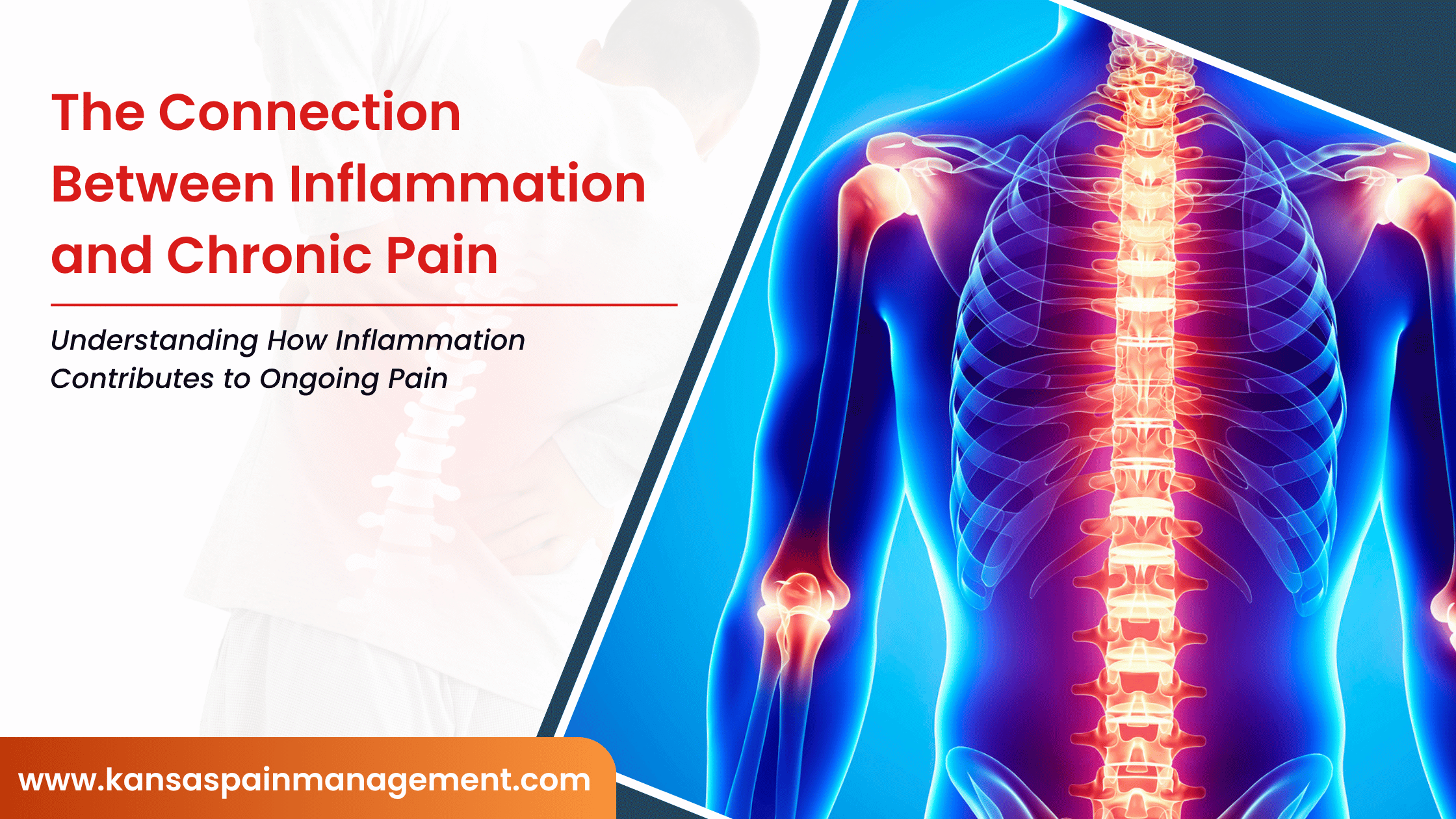
The Brain–Pain Connection
Pain is not just physical—it’s processed in the brain.
When stress levels are high:
- The brain becomes more sensitive to pain signals
- Pain feels stronger and more persistent
- The body becomes more reactive to minor triggers
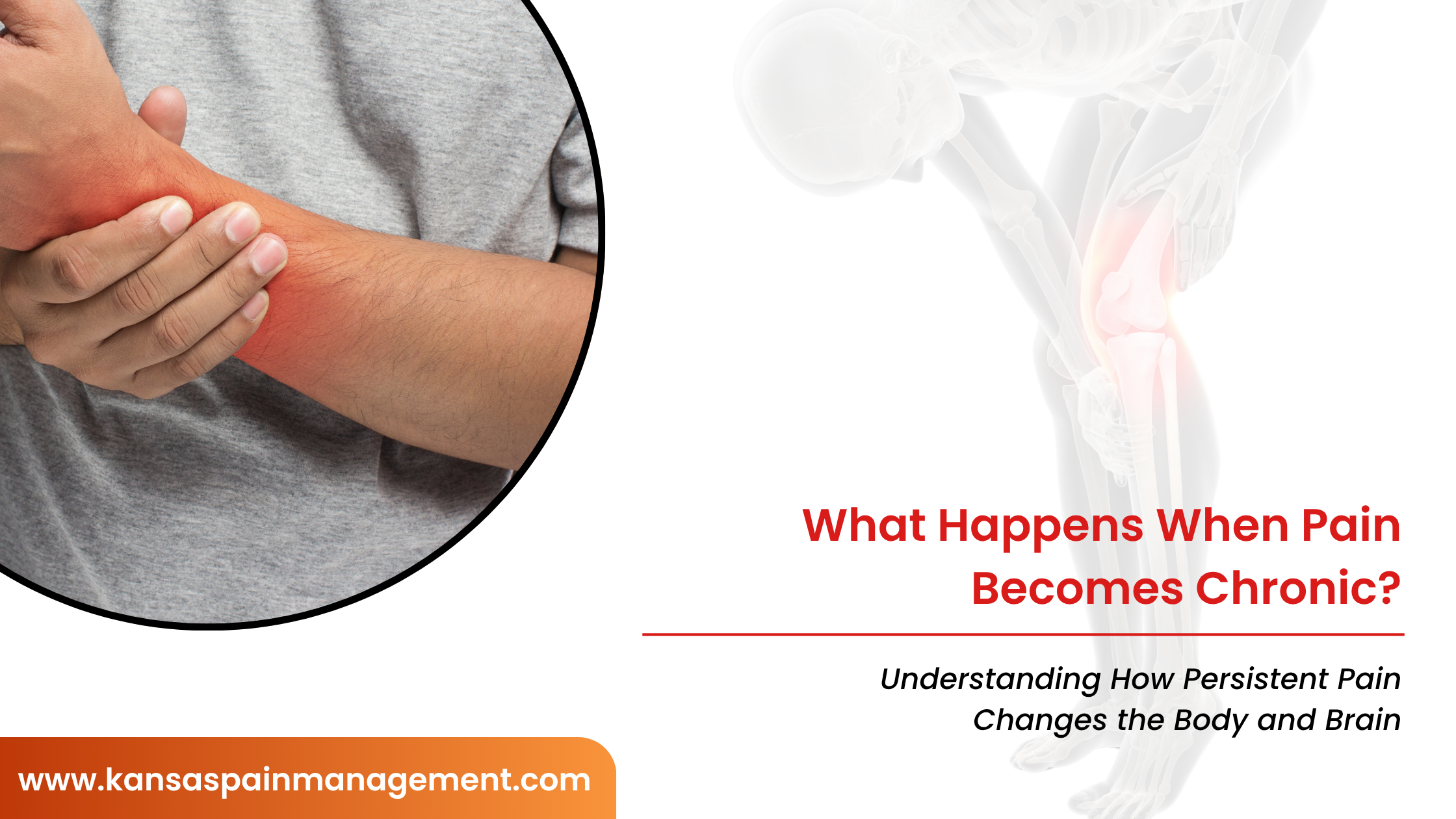
This is sometimes referred to as central sensitization, where the nervous system amplifies pain signals over time.
Why Stress Can Make Pain Feel Worse
1. Increased Muscle Tension
Stress causes muscles—especially in the neck, shoulders, and lower back—to tighten. This can lead to:
- Stiffness
- Reduced mobility
- Increased discomfort
2. Heightened Nerve Sensitivity
Stress can make nerves more reactive, leading to:
- Burning or tingling sensations
- Increased pain intensity
- More frequent flare-ups
3. Poor Sleep
Stress often disrupts sleep, and poor sleep can:
- Slow healing
- Increase inflammation
- Lower pain tolerance
4. Reduced Pain Threshold
When stressed, the body becomes less tolerant of discomfort, making even mild pain feel more severe.
Common Pain Conditions Affected by Stress
Stress can worsen many chronic pain conditions, including:
- Chronic neck and back pain
- Tension headaches
- Migraines
- Fibromyalgia
- Nerve-related pain
Even if the original cause is physical, stress can intensify symptoms.
How to Manage Stress-Related Pain
Managing stress is an important part of pain treatment. Strategies may include:
Relaxation Techniques
- Deep breathing exercises
- Meditation or mindfulness
- Gentle stretching or yoga
Physical Activity
Regular movement helps:
- Reduce muscle tension
- Improve circulation
- Release natural pain-relieving chemicals
Sleep Improvement
Better sleep supports healing and reduces pain sensitivity.
Targeted Pain Treatments
At Kansas Pain Management, interventional treatments can help reduce the physical source of pain, making it easier to manage stress-related symptoms.
Why a Comprehensive Approach Matters
Pain is rarely caused by just one factor. The most effective treatment plans address both:
- Physical causes (joints, nerves, inflammation)
- Neurological factors (how the brain processes pain)
This combined approach leads to better, longer-lasting results.
When to See a Pain Specialist
You may benefit from evaluation if:
- Pain worsens during stressful periods
- Pain persists despite rest or treatment
- You experience frequent flare-ups
- Pain is affecting sleep or daily life
Understanding the connection between stress and pain can help guide more effective treatment.
Taking Control of Pain and Stress
Stress does not mean your pain isn’t real—it means your nervous system may be amplifying the signals.
At Kansas Pain Management, we focus on identifying the underlying causes of pain while helping patients manage contributing factors like stress, posture, and lifestyle.
With the right approach, it’s possible to reduce both stress and pain—and improve overall quality of life.
Schedule a Consultation
If stress seems to be making your pain worse, a comprehensive evaluation can help identify the source and guide effective treatment options.
Contact Kansas Pain Management to learn more about personalized, non-surgical pain relief strategies.