COVID-19 led to sudden and unforeseeable changes in every aspect of our lives. Hospitals and independent medical practices were forced to adapt to rapidly changing safety guidelines and left to make changes based on their individual circumstances. Many private practices faced severe financial difficulties and steadily declining revenues as patients were hesitant to seek medical care.
At the same time, medical practices have an ethical obligation to help slow the spread of COVID while maintaining patient trust and health. Here, we provide a brief example of how Kansas Pain Management – a group of clinics providing comprehensive interventional pain management across three Kansas locations – was able to grow its practice in 2020 despite COVID, something we continue to do in 2021 as well.
COVID Considerations Among People with Chronic Pain
According to a paper published by a team at the University of Arizona in January 2021, COVID-19 infection may “silence” or suppress pain subversion of VEGF-A/NRP-1 signaling, and may explain why so many infected people experience few or no symptoms.1 As a result, infected individuals do not stop their daily activities because they do not feel the symptoms, which heavily contributes to unrelenting community spread. Pain management doctors must take this into consideration when formulating treatment plans and diagnoses.
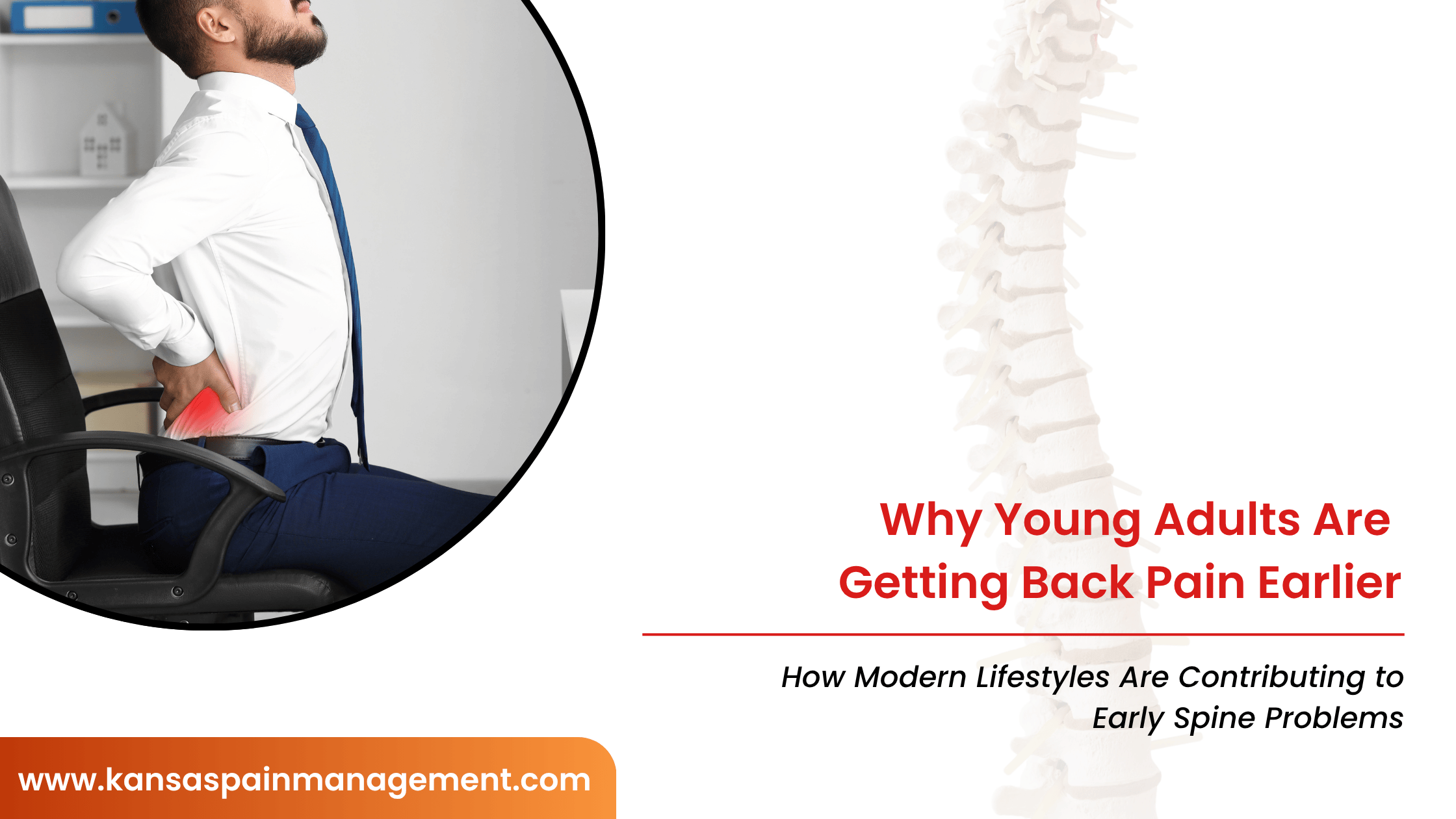
Lockdowns have had a vastly disproportionate negative impact on those with chronic pain. A survey in the United Kingdom investigated how lockdown restrictions affect those with chronic pain as opposed to healthy individuals. Individuals in the studied healthy group experienced no major differences in pain while those with chronic pain experienced a sharp increase in pain symptoms. Furthermore, those with chronic pain demonstrated a worrisome increase in mental health issues, such as anxiety and depression.2 These factors must be taken into consideration when treating patients with chronic pain during the ongoing pandemic.
Our Pain Practice: The Early Phases of the COVID Pandemic
Kansas Pain Management (KPM) understands the importance of helping patients feel secure in getting medical attention and providing a safe environment for healthcare employees while remaining financially viable. When the pandemic hit the United States, KPM immediately responded by:
- canceling elective, nonemergent procedures for a 45-day period
- performing a weekly review of CDC guidelines, state regulations, and local county guidelines
- offering telemedicine appointments, which provided more accessibility to patients, including those in more rural areas
- being aggressive about cleaning – we hired a new environmental service staff to regularly clean rooms at the end of each clinic day
- actively triaging patient appointments and patients to collaboratively determine which patients needed to come in-person for procedures.
The practice team quickly learned that patient education and transparency would be key. That meant providing patients with alternate options for receiving care, such as telemedicine and home-based physical therapy. With a limited number of outpatient procedure slots for patients in severe pain, patients were screened 1 day prior for fever, COVID-19 contact, and history of travel. They were informed about the new check-in procedures, mask requirements, and safety protocols, including the inability for relatives to be in the waiting area.
Initially, some patients refused to wear masks, however, once there was clear direction from the CDC, patients became more amicable. The clinicians and medical staff provided patients with updates and timelines regarding their care, which offered a level of communication that helped patients stay calm and informed.
Long-Term Pandemic Planning and Financial Viability
In-Patient Consults, Office Procedures, Telemedicine, and Drug Monitoring
To accommodate the difficulties associated with the pandemic and implement long-term solutions, physicians from the practice continued to provide in-patient consults to treat hospitalized patients. KPM maintained office procedures for patients with a pain score of 8 out of 10 or higher as long as they cleared the COVID Questionnaire. Our goal was to limit ER visits by these patients, which would a) further overwhelm local hospitals, and b) potentially expose them to COVID.
Although telemedicine seemed like an ideal solution at the beginning of the pandemic, the practice soon realized that telehealth alone did not generate enough revenue to remain financially viable.
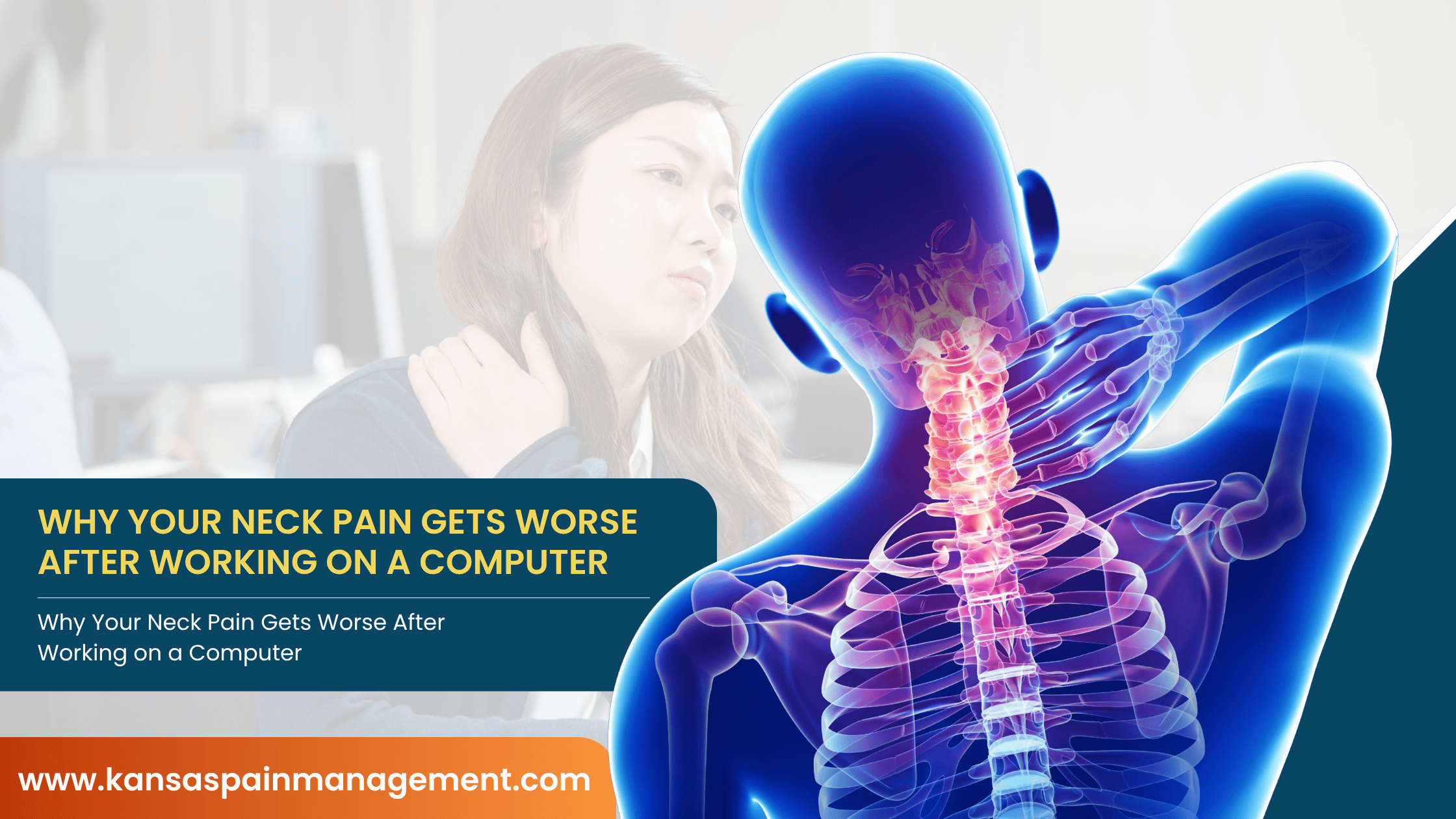
We made the choice to centralize most of our IT and technology services and to focus on learning how to effectively use simultaneous programs such as Zoom, Webex and Doximity. We went into this new type of care with the awareness that telemedicine is not perfect: many households do not have smartphones or adequate Wi-Fi, important physical findings may be missed, interventions cannot be performed, and without urine screens and drug monitoring, drug diversion or abuse may be enhanced. Yet, telemedicine offered the best way to provide safe care to patients at the time; many clinics plan to continue partial use of telemedicine after the pandemic.³
To address drug monitoring, we relied on the state prescription drug monitoring program (PDMP) to assess diversion and doctor shopping. Any opioid prescriptions coming out of our clinics were written on paper which the patient had to pick up from a staff medical assistant, who then ensured the patient was not overly sedated and obtained a urine sample if indicated. However, if the televisit or PDMP revealed any potential red flags, patients were informed that they would need to come and see a provider in person within 5 working days.
Patient Autonomy
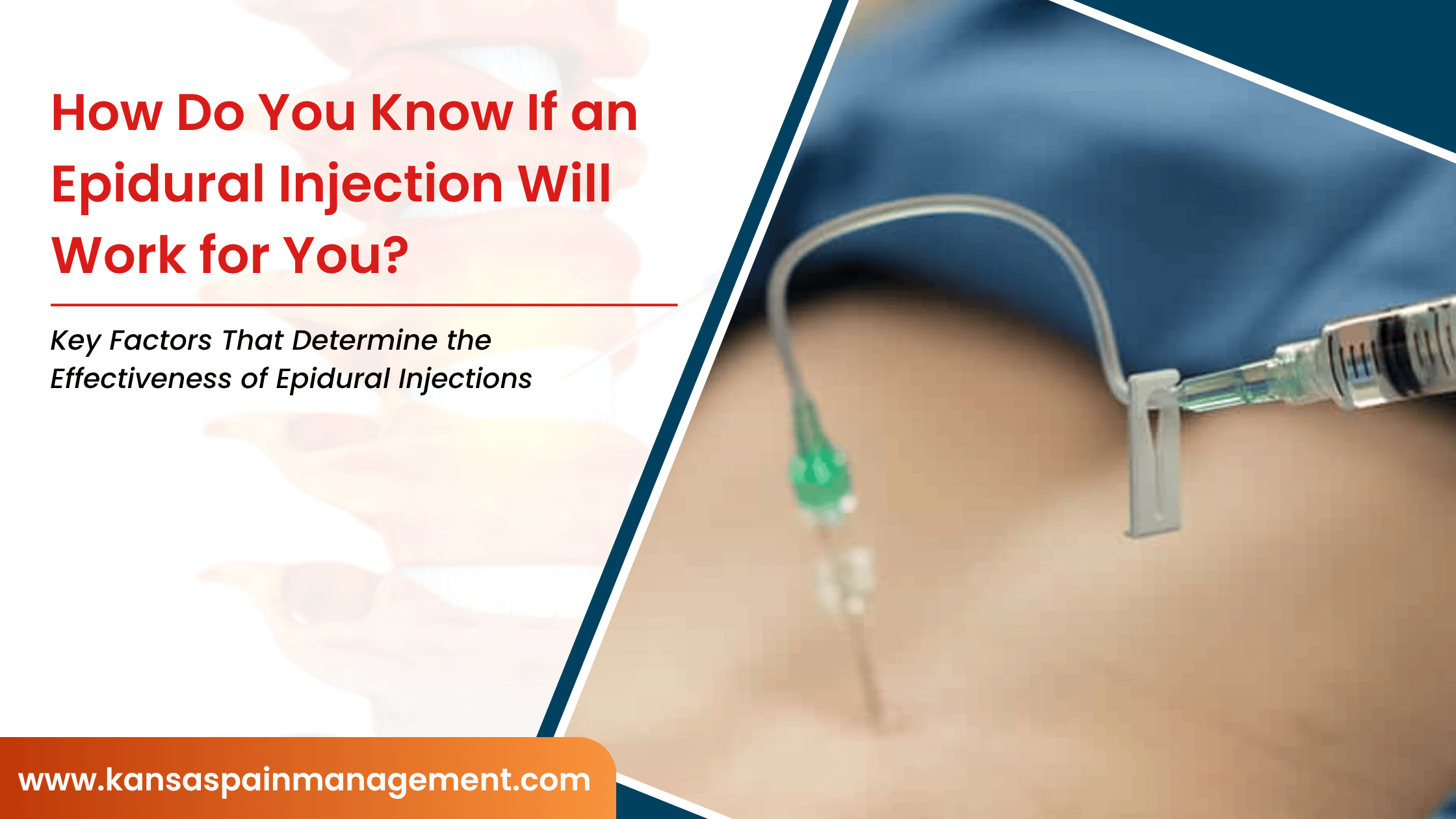
Some interventional procedures could be done safely in our clinics during the pandemic (eg, transforaminal epidurals, facet blocks, and joint injections) but neuromodulation involving peripheral stimulators had to be delayed as all elective procedures were put on hold. Thus, we gave our patients the autonomy to choose whether they would come in person to receive such procedures or delay their treatment.
We analyzed the research data available and measured that with the importance of providing care to patients with chronic pain. With this information, the practice informed patients of the risks associated with each decision, ultimately leaving it up to the individual.
Adapting to New Paperwork Challenges and COVID Safety Protocols
With the new structure of seeing patients virtually and in person, there was more paperwork to be done and appointments were significantly longer than normal. Thorough cleaning before and after each appointment added additional time that had been previously utilized attending to patients.
Additionally, more employees were calling out sick after any potential COVID exposure. It took the practice a few weeks to cope with these changes but, eventually, our new protocols aligned. Patient satisfaction improved and many patients felt safe to return to their regular appointment schedules.
Growth Management
Still, KPM focused on being proactive to keep the practice going and growing strong. Teams scheduled long-term telemedicine follow-ups with established patients to ensure they stayed with the practice and receive continuity of care. We took safety measures recommended by the CDC when seeing severe pain patients in person for procedures. (Since the CDC continually changed its guidelines throughout 2020, the practice looked at previous examples of prevention methods and maintenance of a medical office as well.)
We hired a staff member to determine COVID exposure in the business. This included implementing a process of touchless car check-ins to reduce the amount of time that patients spent in the building. Moreover, to ensure retainment of patients, KPM took steps to increase its social media presence, such as through a Facebook page that provided weekly updates about the practice and which encouraged patients to get the care they deserved while staying safe during the pandemic.3
In the early months of the pandemic, we were fortunate to have implemented telemedicine early on and were wise to close some of our smaller clinics. KPM directed in-person patients to its main office and concentrated staff and equipment there. We sourced PPE from separate vendors to not be in short supply and made these resources available to all staff.
In Summary
Despite all of these changes, KPM did not forget or give up on its long-term vision and continued with expansion plans beginning in June 2020; in some ways, the pandemic provided time to adequately plan for this growth. In the first week of November 2020, we opened a new fourth center in Lawrence, Kansas. Soon after the initial phases of the pandemic, we also reopened our smaller centers for patients who were not able to travel long distances and to maintain social distancing measures in our offices – this contributed to further patient retention. Lastly, we stayed positive.
As front-liners receive their COVID vaccines, the pandemic will still likely push clinicians and medical staff out of their comfort zones, but we believe strongly this will only encourage the advancement of healthcare and pain practice.
Source:-Click here